For ease of reference, figures in brackets refer to the reference numbers appended to this document.
Everyone knows that fiber is «good for you». But did you know that majority of people are not meeting their daily needs. According to data collected in 2004 during the’Canadian Community Health Survey, women consumed between 15.5 and 17.5 g of fibre per day, and men between 18 and 21 g (7), whereas the recommended daily fibre intake for adult women is 25 g and for adult men 38 g (12).
What's more, did you know that not all fibers are the same? different roles and functions?
It will help you understand their implications for overall health, their characteristics and their uses in clinical nutrition!
Definition and food sources
Fibers are defined as polymers of carbohydrates that are neither digested nor absorbed, and are subject to fermentation by bacteria in the gastrointestinal tract (5, 6). They have an impact on the composition of the microbiota's bacteria and its metabolic activities (6).
Here are the main sources of dietary fibre (11):
- Vegetables
- Fruits
- Pulses: e.g. chickpeas, beans, lentils
- Nuts and seeds: e.g. almonds, walnuts, sunflower and pumpkin seeds
- Flax and chia seeds
- Whole-grain products: whole-grain cereals and breads, brown rice, hulled barley, whole oats, buckwheat
Many benefits
Fiber intake is recommended for a number of reasons. In multiple observational studies, fiber intake has been associated with reduced risk and mortality for several health conditions such as; cardiovascular disease, obesity, diabetes and colon diseases such as colorectal cancer and diverticulitis (4, 5, 8). For example, oat fibre (ß-glucan) reduces blood cholesterol and improves glycemic (blood sugar) control (5, 8). From intestinal side, Fiber promotes intestinal motility and regularity, as well as a «healthy» microbiota (8, 9).
Health benefits attributed to fiber (8):
↓ blood glucose levels
↓ post-prandial glucose and insulin levels (after meals)
↓ total and LDL («bad») cholesterol levels
↓ blood pressure
↓ energy intake by increasing satiety
↓ intestinal transit time
↑ mineral absorption in the intestine
The daily recommendation for adults varies according to gender (12)
| Gender | Age | Fibre recommendations per day |
| Men | 19-50 years 51 and over |
38 g 30 g |
| Women | 19-50 years 51 and over |
25 g 21 g |
Recommendations of between 25 and 30 g of fiber per day are based primarily on their effect on intestinal regularity and cardiovascular health (8). However, these recommendations have been called into question in various scientific articles (8). Indeed, to maximize their benefits, some authors and organizations advocate the recommendation of 50 g per day (5, 8). For example, some authors mention that this amount is necessary to support colon health and eliminate biomarkers of colorectal cancer risk (5,8).
You're curious to know if you're getting enough fiber: this fiber calculator can help you.
Effect on microbiota
In addition to the many benefits mentioned above, fiber plays a beneficial role in the health of the intestinal microbiota. In fact, fiber is a substrate (food) for the microbiota, promoting the production of’short-chain fatty acids (AGCC) (3, 10). A high-fiber diet has been associated with increased production of SCFAs in the gut, and an increase in «beneficial» bacteria such as Lactobacillus and Bifidobacteria (2, 3). SCFAs include acetate, propionate and butyrate. They have an important effect on the gut microbiota, since between 90 and 99% of SCFAs are absorbed in the gut or utilized by the microbiota (6).
Examples of the role of short-chain fatty acids (SCFAs) (5, 6, 8):
- Energy source for colonocytes (epithelial cells of the colon) and enterocytes (epithelial cells of the intestine)
- Impact on the integrity (quality) of gastrointestinal epithelial cells
- Improved mucus production and secretion
- Involved in glucose (blood sugar) homeostasis (maintenance and stability)
- Involvement in lipid (fat) metabolism
- Effect on appetite regulation
- Involvement in immune function
- Anti-inflammatory effect
The impact of fiber on the microbiota is very real and even at high speed (6). Changes in bacterial diversity and fermentation products were demonstrated in just 24 hours in humans switching from a high-fiber diet (> 30 g) to a fiber-free meat-based diet (6).
What's more, some fibers are classified as prebiotics such as fructan and inulin (6, 8). Not all fibers are prebiotics, but the majority of prebiotics are dietary fibers (6). Prebiotics are defined as fermented ingredients that induce specific changes in the composition and/or activity of the intestinal microbiota, conferring health benefits on the host (5, 6). In a systematic review and meta-analysis of 64 randomized controlled studies in humans, it was observed that fibers, particularly fructans and galacto-oligosaccharides (GOS) and other prebiotic fibers, increased the abundance of Bifidobacterium and Lactobacillus, two «beneficial» bacteria (5).
Although the microbiota can be influenced by fiber and prebiotic intake, different effects have been observed between individuals (6). Individualized recommendations is essential, since every microbiota is unique!
Fiber characteristics
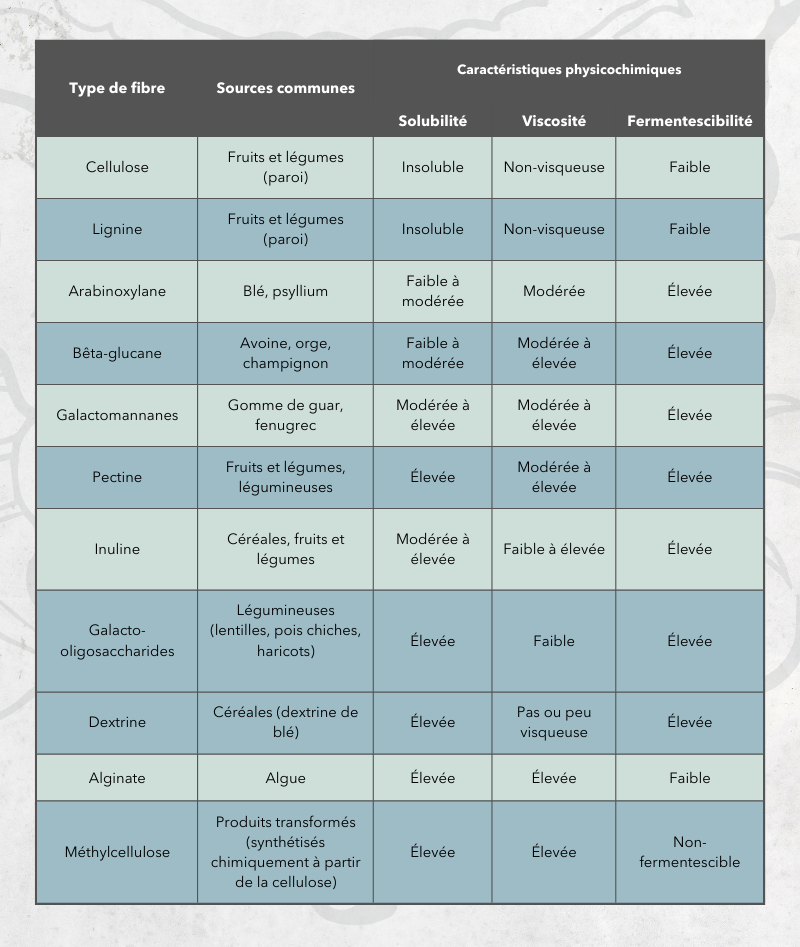
Obviously, depending on the different food sources, fibers vary according to their chemical composition and physicochemical properties such as solubility, viscosity and fermentability (6).
Solubility
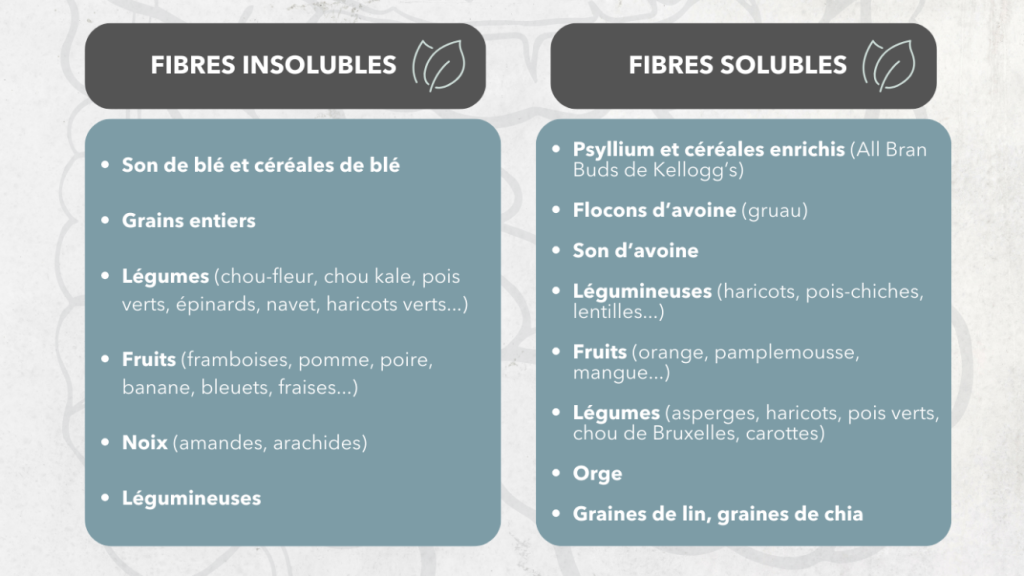
Solubility refers to the extent to which fiber can dissolve in water (5). There are two types of fiber in the diet: soluble and insoluble.
→Soluble fibers: mix with water, creating a gel-like substance that is digested by bacteria and improves stool viscosity (texture) (3, 9)
→Insoluble fibers: reduce intestinal transit time, stimulate contractility and increase stool volume (3, 5, 6, 9)
Dietary sources of soluble and insoluble fibre
Viscosity
Viscosity is the degree of flow resistance, i.e. the ability of a fiber, when hydrated, to thicken as a function of concentration (5). For example, pectins have the ability to form gel networks (5) and are often used in recipes such as jam. It has been suggested that increasing the luminal viscosity of the gut has multiple health benefits (5). Indeed, consumption of viscous dietary fibers modifies transit time in the upper intestine, notably by decreasing gastric emptying rate and modulating small intestinal transit (5). This increase in luminal viscosity plays a role in the above-mentioned beneficial effects of fiber, notably by delaying digestion, lowering blood sugar and cholesterol absorption, and increasing satiety (5).
Fermentability
Fibers may or may not be fermentable, and their degree of fermentability varies from one food source to another (5). The speed at which fibers ferment varies from one type of fiber to another. It is this fermentation that is often blamed for gastrointestinal discomforts such as gas and bloating. This concept also refers to the FODMAP approach, which aims to reduce fermentable foods to help manage gastrointestinal symptoms (3, 5). To find out more about this approach, see the blog article Irritable bowel syndrome: Beyond FODMAPs, what are the different avenues of intervention?
Adapted from Gill et al (2021) (5)

Adapted from Gill et al (2021) (5)
Intestinal diseases and fiber
Irritable bowel syndrome (IBS), often referred to as irritable bowel syndrome.
As mentioned above, not all types of fibre have the same effect on the intestines. Adjustment of choice, distribution and quantity are determined by the symptoms reported. The blog Irritable bowel syndrome: Beyond FODMAPs, what are the different avenues of intervention? describes all the elements of IBS very well.
Visit insoluble fibers are generally more fermentable and may contribute more to digestive discomforts in the context of IBS, such as bloating and abdominal pain (3, 5). For their part soluble fibers are most associated with benefits in relieving IBS symptoms by reducing bloating, flatulence and abdominal distension (1, 3, 4). Psyllium, for example, has beneficial effects on overall IBS symptoms (1, 3, 4). Several publications recommend the consumption of 2 tablespoons (30 ml) per day of ground flaxseed to help manage intestinal symptoms in IBS (4). In addition, fiber is necessary in the presence of constipation by increasing stool volume and frequency (5). To find out more about diarrhea, see the Blog Daily diarrhoea: what can help?
Inflammatory bowel diseases (IBD): Crohn's disease, ulcerative colitis
Studies report that people with inflammatory bowel disease (IBD) such as Crohn's disease or ulcerative colitis consume less fibre than the general population (8). This may be due, in part, to certain medical recommendations to reduce fiber intake (8). On the other hand, the scientific literature is still mixed on the clinical benefits of fiber in IBD (5). Some of the mechanisms considered to explain potential benefits would be SCFAs, which may attenuate intestinal inflammation (5). Thus, according to current studies, fiber is not necessary to restrict during IBD, unless there is a risk of possible intestinal obstruction (5). Of course, fibre tolerance may vary between the active and remission phases of the disease (5). A nutritionist can help you manage your fibre intake according to the activity of your disease.
Diverticulitis
In several prospective studies (subjects followed over time), the risk of diverticulitis was reduced as fibre intake increased (5). Conversely, prospective studies have found an increased risk of diverticulitis with low fiber intake (5). Possible explanations that fiber reduces the risk of diverticulitis are increased stool volume, reduced colonic pressure and reduced herniation (5). The target intake seems to be between 20 and 30 g per day, but further studies are needed to confirm this (5). Fiber restriction seems to be necessary in the very short term for «active» diverticulitis, but this is still «up for debate» by science (5).
What about supplements?
Various studies have found an overall improvement in intestinal symptoms when taking fiber supplements (9). The benefits observed were significant when psyllium (vs. control group) (1,9). A wheat supplement, on the other hand, showed no significant effect on intestinal symptoms (1,9). Depending on your symptoms and dietary habits, fiber supplements may be considered (e.g. psyllium, partially hydrolyzed guar gum, ground flaxseed). Find out more about the different uses of certain fiber supplements, this course may be of interest to you.
In conclusion, fiber has many benefits for overall health, especially intestinal health! Eating fiber is essential. I hope I've convinced you to eat a little more of it, through a colorful and diversified diet.
References
(1) American Gastroenterological Association (AGA) Chey WD, Hashash JG, Manning L, Chang L. AGA Clinical Practice Update on the Role of Diet in Irritable Bowel Syndrome: Expert Review. Gastroenterology. 2022 May;162(6):1737-1745.e5. https://pubmed.ncbi.nlm.nih.gov/35337654/
(2) Beam A, Clinger E, Hao L. Effect of Diet and Dietary Components on the Composition of the Gut Microbiota. Nutrients. 2021 Aug 15;13(8):2795. https://pubmed.ncbi.nlm.nih.gov/34444955/
(3) El-Salhy M, Ystad SO, Mazzawi T, Gundersen D. Dietary fiber in irritable bowel syndrome (Review). Int J Mol Med. 2017 Sep;40(3):607-613. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5548066/
(4) Galica AN, Galica R, Dumitrașcu DL. Diet, fibers, and probiotics for irritable bowel syndrome. J Med Life. 2022 Feb;15(2):174-179. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8999090/
(5) **Gill SK, Rossi M, Bajka B, Whelan K. Dietary fibre in gastrointestinal health and disease. Nat Rev Gastroenterol Hepatol. 2021 Feb;18(2):101-116. https://pubmed.ncbi.nlm.nih.gov/33208922/
(6) Holscher HD. Dietary fiber and prebiotics and the gastrointestinal microbiota. Gut Microbes. 2017 Mar 4;8(2):172-184. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5390821/
(7) Institut national de santé publique du Québec (INSPQ), La consommation alimentaire des adultes québécois selon le poids corporel, 2011. https://www.inspq.qc.ca/publications/1364
(8) McKeown NM, Fahey GC Jr, Slavin J, van der Kamp JW. Fibre intake for optimal health: how can healthcare professionals support people to reach dietary recommendations? BMJ. 2022 Jul 20;378:e054370. https://pubmed.ncbi.nlm.nih.gov/35858693/
(9) Patel NV. «Let Food Be Thy Medicine: Diet and Supplements in Irritable Bowel Syndrome. Clin Exp Gastroenterol. 2021 Sep 22;14:377-384. https://www.niddk.nih.gov/health-information/digestive-diseases/irritable-bowel-syndrome/eating-diet-nutrition
(10) Rinninella E, Tohumcu E, Raoul P, Fiorani M, Cintoni M, Mele MC, Cammarota G, Gasbarrini A, Ianiro G. The role of diet in shaping human gut microbiota. Best Pract Res Clin Gastroenterol. 2023 Feb-Mar;62-63:101828. https://pubmed.ncbi.nlm.nih.gov/37094913/
(11) Health Canada Fibre Page consulted online: https://www.canada.ca/fr/sante-canada/services/nutriments/fibres.html
(12) Health Canada Tables of Dietary Reference Intakes: Reference values for macronutrients Page consulted online : https://www.canada.ca/fr/sante-canada/services/aliments-nutrition/saine-alimentation/apports-nutritionnels-reference/tableaux/valeurs-reference-relatives-macronutriments.html